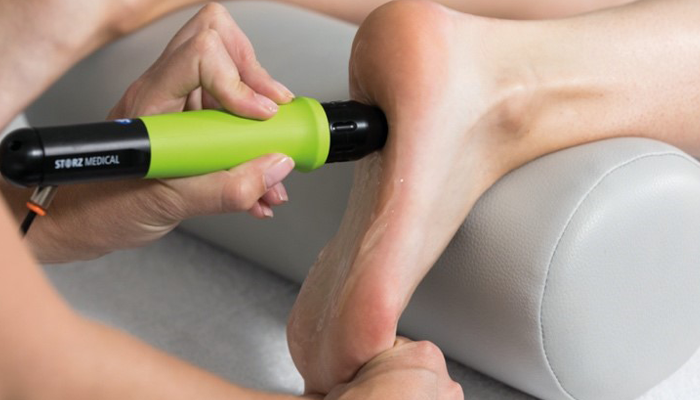
Plantar Fasciitis Relief in Murray, Utah
That sharp heel pain with your first few steps in the morning? The ache under your heel after a run on the Jordan River Trail, climbing Grandeur Peak in Millcreek, hiking the Cottonwoods, or simply being on your feet all day at work? Plantar fasciitis is one of the most common foot injuries we help runners and active adults overcome at Revive Sport & Spine.
For many people, it starts subtly with mild soreness after a run, tenderness after a long day, or discomfort walking barefoot at home. Then suddenly it becomes the thing you think about every morning, every workout, and every step after sitting too long.
At our Murray sports chiropractic clinic, we help active adults in Murray, Holladay, Cottonwood Heights, Midvale, and Sandy get back to running, lifting, hiking, golf, and daily life with a treatment plan built around soft tissue therapy, shockwave therapy, foot and ankle mobility, and progressive exercise rehabilitation.
The good news: most cases improve very well with the right conservative plan, and many people begin noticing meaningful progress within 6–8 weeks. Our aim at Revive Sport & Spine is to enable faster recovery through shockwave therapy and adherence to in-clinic and home rehabilitation exercises.
Our goal is not just short-term symptom relief. We want to identify why your plantar fascia became overloaded in the first place; whether that is calf tightness, poor ankle mobility, foot weakness, training progression, or running mechanics, so you can recover fully and reduce the risk of it returning.
If heel pain is already changing how you run, walk, train, or recover, the sooner we address the true driver, the faster we can help you get back to doing what you love.
What is Plantar Fasciitis?
The plantar fascia is a thick, fibrous band of tissue that runs from your heel bone to the base of your toes, helping support the arch of the foot and act like a built-in spring every time you walk, run, hike, or lift. Its job is to help your foot absorb force, stiffen during push-off, and efficiently transfer energy forward—especially during running and other repetitive activities. Your TRF guide explains this really well through the arch support role and the windlass “spring” effect during push-off.
For runners and active adults, this tissue takes on a tremendous amount of repetitive load. Every stride, hill, speed workout, long walk, pickleball match, or day spent on your feet adds stress to the plantar fascia. When the calf is tight, ankle mobility is limited, the big toe does not extend well, or the foot and hip muscles are not doing their job, the stress can become concentrated at the point where the fascia attaches near the heel.
Despite the name, research suggests plantar fasciitis is usually less of a true inflammatory condition and more of a chronic tissue overload problem with degenerative changes in the fascia. This is why terms like plantar fasciopathy or plantar heel pain are becoming more common in the literature.
This distinction matters because it explains why complete rest, ice alone, or simply waiting it out often only gives temporary relief. The pain may calm down for a short time, but if the foot, calf, ankle, and overall movement system are not better prepared to handle load, symptoms often return as soon as running, long walks, hiking, or workouts increase again.
It is also important to note that not all heel pain is due to plantar fasciitis. Fat pad irritation, Achilles-related pain, nerve irritation, posterior tibialis dysfunction, or even a heel stress reaction can create symptoms that feel very similar. This is why a thorough exam matters. At Revive Sport & Spine, we assess foot mechanics, ankle mobility, calf strength, training history, footwear, and movement patterns to identify the true driver and guide the right treatment from day one.
This understanding shapes our treatment philosophy: rather than just chasing pain or inflammation, we focus on restoring mobility, improving tissue load tolerance, and rebuilding the strength your foot needs to handle real life again.
Common Symptoms of Plantar Fasciitis
Plantar fasciitis symptoms often start subtly and gradually become more noticeable over a few days to weeks. While every case is a little different, the most common symptoms we see in runners and active adults include:
Sharp heel pain with your first few steps in the morning
Pain at the bottom or inside of the heel
Heel pain after sitting for long periods, then standing up
Pain during the first mile of a run that may ease as you warm up
Symptoms that return after longer runs, hikes, pickleball, or long days on your feet
Increased pain when walking barefoot on hard floors at home
Tenderness when pressing on the inside bottom portion of the heel
Tight calves, stiff ankles, or poor big toe mobility
Pain that feels worse the day after a harder workout or long walk
Heel discomfort that changes the way you walk, run, or stand
A pulling or tight sensation through the arch of the foot
Pain that improves temporarily with rest but quickly returns when activity picks back up
Because not all heel pain is plantar fasciitis, symptoms such as burning, numbness, tingling, bruised-feeling heel pain, or pain higher up in the Achilles or calf may point to a different issue and should be properly evaluated.
At Revive Sport & Spine, one of the biggest goals of the exam is determining whether your symptoms are truly coming from the plantar fascia, or whether another structure is creating similar heel pain and leading you toward the wrong treatment.
Why Plantar Fasciitis Occurs:
Plantar fasciitis usually develops when the load placed on the plantar fascia exceeds the tissue’s current capacity. In other words, the demands of running, hiking, standing, or daily activity increase faster than the foot, calf, and lower body are prepared to handle.
For runners and active adults, the most common contributors include:
The “Terrible Too’s” — Too Much, Too Fast, Too Hard, Too Soon
One of the most common drivers we see in runners is a rapid increase in mileage, speed work, hill training, or race-specific intensity. When volume and intensity increase faster than tissue capacity, the plantar fascia is often among the first structures to become irritated.Limited Ankle Mobility
Poor ankle dorsiflexion is one of the biggest contributors to plantar fascia overload. When the ankle cannot move forward efficiently, more stress is transferred into the arch and heel during walking and running.Restricted Big Toe Mobility
The plantar fascia relies heavily on the big toe extending properly during push-off. If the toe is stiff, the foot loses its natural spring mechanism, and more tension builds near the heel.Poor Warm-Up and Mobility Habits
Many runners jump straight into their run, barely warm up, and only stretch when something starts hurting. Better foot, calf, ankle, and hip mobility habits often make a huge difference in both recovery and prevention.Improper Running Mechanics
Hip adduction and knee internal rotation, which many runners notice as the knee collapsing inward, can change how the foot loads the ground and increase stress through the arch and plantar fascia.Tight or Weak Hip Musculature
While the pain is in the foot, the real driver is often higher up the chain. Weak hips, poor pelvic control, and limited lateral hip stability can all create excessive foot stress with every stride.Calf Tightness or Weakness
The calf complex plays a major role in absorbing and transferring force. When it lacks mobility or strength, the plantar fascia may have to take on more of that workload.Lack of Training Variety
Using the same pace, same shoes, same route, and same terrain every day can overload the same tissues repeatedly. Mixing in trails, shorter runs, intervals, hills, recovery runs, and strength work helps spread stress more effectively.
For active adults who are not runners, we commonly see plantar fasciitis triggered by:
Long hours standing at work
Sudden increases in walking or activity
Hiking, especially on downhill or uneven terrain
Walking barefoot on hard floors
Weight gain or reduced recovery capacity with age
Poorly supportive daily footwear
This is why treatment should never focus on the foot alone. At Revive Sport & Spine, we look at the entire movement chain, from the hips to the ankle to the big toe, to identify the real reason the plantar fascia became overloaded in the first place.
Our Plantar Fasciitis Treatment Approach at Revive Sport & Spine
At Revive Sport & Spine, our goal is to do more than just calm heel pain; we want to identify why it started, treat the irritated tissue, and rebuild the strength and movement capacity needed to keep you active long term.
Our treatment process is designed to help runners and active adults in Murray, Utah, return to training, hiking, golf, pickleball, and daily life with as little disruption as possible.
Step 1: History + Training Review
Every plantar fasciitis case starts with understanding the full story. We will review recent changes in mileage, hiking, walking, or workouts; terrain changes, such as trails, hills, or treadmill-to-road transitions; footwear and barefoot habits; work demands and time spent standing; previous calf, Achilles, or foot issues; and how symptoms respond during and after activity. This often reveals the true reason the plantar fascia became overloaded.
Step 2: Detailed Movement + Foot Exam
We do not just look at the painful heel. Your exam includes: plantar fascia tenderness and tissue loading; ankle dorsiflexion mobility; big toe extension; calf mobility and strength; intrinsic foot strength and balance; hip mobility, stability, and strength; and gait and running mechanics when needed. This helps us determine whether the issue is truly plantar fasciitis—or another heel pain source that needs different treatment.
Step 3: Hands-On Treatment + Shockwave
Once we confirm the diagnosis, we begin treatment right away. This commonly includes:
Shockwave Therapy, often starting in the first 1-2 visits
Soft Tissue Treatment for the plantar fascia, calf, Achilles, and surrounding lower leg structures, which may include IASTM and dry needling therapy.
Joint Mobilization for the ankle, foot, and big toe to restore normal motion
For most cases of plantar fasciitis, we recommend 6–8 shockwave sessions, with longer-standing cases sometimes needing additional support. This can be affected by your attention to and frequency of home care exercises, as well as adherence to training and lifestyle modifications.
Step 4: Strength + Exercise Rehabilitation
In-office and home strength and stability rehab exercises are where long-term results happen. Skipping this step will leave you frustrated and wondering why you just can’t get rid of this foot pain. Simply put, we have to build up the tolerance of your feet and lower legs to handle the stress of the activities you want to do. We start with focused foot, ankle, and calf loading, then as symptoms improve, we progress from smaller foot-specific exercises into larger hip and stance-dominant strength work that better reflects real-life activity and running.
Step 5: Training + Lifestyle Modifications
When working through plantar fasciitis or any other injury, we are generally aggressive about keeping you active as long as the tissue is responding well. In most cases, we aim to maintain running, hiking, lifting, or walking with:
pain kept at 3/10 or less
a temporary 30–50% reduction in total volume
lower exercise intensity early with hills and speed work reintroduced later
home mobility and calf work performed frequently
footwear and barefoot habits adjusted as needed
Home care is one of the biggest predictors of how quickly this improves.
Step 6: Gradual Return to Unrestricted Activity
Our final phase is to build confidence and durability so you can return to unrestricted running, long hikes in Millcreek and the Cottonwoods, pickleball and other court sports, lifting and gym work, and pain-free daily activity. The goal is not just to feel better, it is to give your foot and lower body the capacity to handle the demands of the activities you actually love.
This is why so many plantar fasciitis cases improve faster when we combine shockwave therapy, hands-on treatment, mobility restoration, and progressive strengthening, rather than relying on passive treatment alone.
Why Shockwave Helps Plantar Fasciitis
Shockwave therapy is one of our most effective treatments for plantar fasciitis, especially when symptoms have become chronic, failed to improve with traditional physical therapy and chiropractic care, returned after steroid injections, or are beginning to ramp up enough to threaten your training.
At Revive Sport & Spine, we often introduce shockwave therapy during the first 1-2 visits because plantar fascia tissue tends to respond very well when combined with the right loading program and movement restoration.
Shockwave helps in three important ways:
Reduces pain sensitivity by calming down the irritated tissue and reducing the morning “first step” pain that makes plantar fasciitis so frustrating.
Stimulates tissue healing + remodeling - Because plantar fasciopathy is more of a chronic tissue overload problem than an inflammatory one, shockwave helps stimulate circulation, collagen remodeling, and the body’s natural healing response in the degenerative fascia tissue.
Improves the tissue’s ability to tolerate load again. Our real goal is to help the plantar fascia better handle running, hiking, lifting, pickleball, and long workdays, not just temporarily numb symptoms.
Many patients begin to notice improvement in just a few visits, especially with reduced first-step morning pain, less discomfort after runs or long walks, better tolerance for standing and daily activity, and improved confidence returning to training.
This is especially helpful for:
chronic plantar fasciitis lasting more than 6 weeks
cases that failed PT, rest, or steroid injections
runners wanting to stop increasing heel pain before it interrupts marathon or race prep
active adults frustrated by recurring flare-ups
One of the biggest benefits is that shockwave offers an effective, research-backed treatment option with no pills, no injections, and no invasive procedures. At the same time, it is not a magic fix. The best outcomes happen when shockwave is paired with calf strength, foot loading, ankle mobility, and smart training modification.
Recent research strongly supports this approach. A 2024 systematic review found that shockwave therapy improved pain, plantar fascia thickness, and foot function better than corticosteroid injections at both 3 and 6 months, making it one of the strongest conservative treatment options available for plantar heel pain.
For many runners and active adults in Murray, Utah, this becomes the turning point that allows them to keep moving forward instead of constantly restarting the recovery and training process.
Who Gets Plantar Fasciitis
Plantar fasciitis can affect both athletes and non-athletes, but certain people are at a much higher risk of developing heel pain. The most common higher-risk groups include:
Adults between 40 and 60 years old
This is the most common age range, likely due to reduced tissue elasticity, calf stiffness, recovery limitations, and the cumulative effects of years of loading.Runners and active adults who are increasing their training load
Marathon prep, spring race season, sudden hill work, speed sessions, big hiking weekends, and big mileage jumps can all rapidly overload the plantar fascia.People with a higher BMI or recent weight gain
Increased body mass increases the repetitive load through the heel and plantar fascia with every step, especially during long standing and walking.Occupations with prolonged standing or walking
Teachers, nurses, warehouse workers, retail workers, healthcare providers, coaches, and anyone standing on hard floors for long periods are at significantly greater risk.People with a previous history of foot, calf, or Achilles pain
Prior plantar fasciitis, Achilles tendinopathy, chronic calf tightness, or recurring foot pain often means the tissue capacity issue was never fully addressed.Those with limited ankle or big toe mobility
Reduced ankle dorsiflexion and poor big-toe extension can dramatically increase plantar fascia stress during walking, stair climbing, and running.
For Runners and Athletes, Risk Increases Further With:
training errors and the “Terrible Too’s” - doing too much, too soon, too fast, too hard, with too little tissue capacity
improper or worn-out footwear
inadequate recovery between hard sessions
sudden speed or hill work
lack of strength training
poor warm-up habits
calf and lower leg fatigue due to strength limitation
The common thread is simple: the load placed on the plantar fascia begins to exceed what the tissue is prepared to tolerate.
The good news is that most of these risk factors are highly modifiable, and with the right exam, shockwave treatment, mobility work, and progressive strength plan, we can not only get back to the activities we enjoy but also prevent future issues.
When Should I Get My Foot Pain Evaluated?
The best time to get plantar heel pain evaluated is before it starts changing how you move, train, or live day to day. We recommend getting it checked sooner if you notice:
Pain is getting worse instead of gradually improving
Morning first-step pain is becoming more intense
Symptoms return every time you try to increase mileage, hiking, walking, or gym activity
Heel pain is beginning to disrupt marathon prep, race training, hiking, golf, or pickleball
Pain worsens as you run instead of easing after warming up
Symptoms are still lingering the next day after activity
You are changing your stride, limping, or avoiding push-off
Walking is becoming painful, not just running
You cannot tolerate hills, speed work, or longer time on your feet
Rest helps temporarily, but symptoms return as soon as activity picks back up
It is also important to get examined if symptoms include:
burning, numbness, or tingling
bruised-feeling heel pain
pain higher into the Achilles or calf
pain with hopping or single-leg loading
night pain
sudden sharp pain or a popping sensation
pain with squeezing the heel bone
These symptoms may suggest something other than plantar fasciitis, such as fat pad irritation, nerve involvement, Achilles referral, or a bone stress injury, and they need to be ruled out with a proper exam. The good news is that earlier treatment almost always means a faster return to the activities you enjoy the most. When plantar heel pain is ignored or treated with rest alone, it often becomes a frustrating cycle that returns every time training ramps up.
At Revive Sport & Spine, our goal is to give you a clear next step so you can maintain as much activity as safely possible and get back to running, hiking, lifting, and daily life quickly and confidently.
Plantar Fasciitis FAQs
Should I stop running with plantar fasciitis?
Not always. At Revive Sport & Spine in Murray, Utah, we try to keep runners active whenever it is safe to do so. In many cases, a 30–50% reduction in running volume, lower intensity, and avoiding hills or speed work early allows healing while maintaining fitness. The key is to keep pain at 3/10 or less and ensure symptoms are not worse the next day.
Will shockwave help plantar fasciitis?
Yes, shockwave therapy is one of the most effective conservative treatments for plantar fasciitis, especially in chronic cases or when symptoms return after PT or steroid injections. Research shows ESWT improves pain and function better than corticosteroid injections at 3 and 6 months, making it one of the strongest evidence-based options available. At Revive, we pair shockwave with hands-on care and strength rehab for the best results.
How long does plantar fasciitis take to heal?
Most people begin to notice improvement within a few visits, especially when shockwave therapy, mobility work, and strength rehab are started early. Research and clinical guidelines suggest that most cases improve significantly within 6-8 weeks, while longer-standing cases may take 2-3 months or longer, depending on training demands and consistency with home care.
Will plantar fasciitis come back?
It can if the real cause is not addressed and home care is not maintained. This is why rest alone often leads to a frustrating cycle where heel pain returns every time mileage, hiking, or daily activity increases. At Revive, we focus on the key contributors: ankle mobility, calf strength, foot stability, hip control, and training progression, to reduce the risk of recurrence and improve long-term tissue capacity.
Stretching isn’t helping. What else should I do?
Stretching alone rarely solves plantar fasciitis because the issue is usually tissue overload and reduced load tolerance, not just tightness. Most people also need: calf and foot strengthening, ankle and big-toe mobility, shockwave therapy, soft-tissue treatment, activity modification, and adjustments to running or walking loads. This is why a full exam often helps people recover much faster than continuing to stretch and hope it improves.
Why didn’t rest work for my plantar fasciitis?
Rest may temporarily calm symptoms, but it does not improve the plantar fascia’s ability to tolerate load. Once running, hiking, standing, or gym activity resumes, the tissue is often not better prepared to handle stress. The most effective recovery plans combine load management, progressive strengthening, mobility restoration, and tissue treatment rather than rest alone.
Why did it come back after PT?
Recurrent plantar fasciitis often means the full movement chain was never addressed. The foot may feel better temporarily, but if ankle stiffness, calf weakness, hip mechanics, training errors, or return-to-running progression were missed, symptoms can easily return. This is why our Murray sports chiropractic clinic looks beyond the heel itself.
Why didn’t the steroid injection fix it?
Steroid injections can reduce pain short term, but they do not improve tissue strength, mobility, or load tolerance. Research suggests ESWT often outperforms corticosteroid injections at mid-term follow-up for plantar heel pain, which is why we often recommend shockwave plus rehab instead of relying on repeated injections.
Do I need an X-ray or an MRI?
Not usually. Plantar fasciitis is most often diagnosed through a detailed history and physical exam. Imaging may be helpful if symptoms suggest a bone stress injury or nerve involvement. At Revive Sport & Spine, we help determine when imaging is actually necessary instead of ordering it automatically.
Is this caused by a heel spur?
Rarely! Research shows that many people have heel spurs without pain, and many cases of plantar fasciitis occur without a spur. The pain is usually more related to plantar fascia overload, stiffness, and tissue degeneration than the presence of a spur itself. Research also shows that foot pain often persists after spur removal.
Get Expert Plantar Fasciitis Treatment in Murray, Utah
If heel pain is starting to affect your running, hiking, workouts, long workdays, or even your first few steps in the morning, the sooner we identify the true driver, the faster you can get back to doing what you love.
At Revive Sport & Spine, we help runners and active adults recover from plantar fasciitis with a clear, step-by-step plan built around shockwave therapy, hands-on treatment, mobility restoration, strength rehab, and smart activity modification, all designed to keep you moving as safely as possible.
Whether your goal is to keep marathon training on track, get back to long hikes in Millcreek and the Cottonwoods, stay pain-free through pickleball season, or simply walk through your day without thinking about your heel, we are here to help.
Our Murray, Utah, clinic proudly serves active adults and athletes from Murray, Holladay, Cottonwood Heights, Millcreek, Midvale, Sandy, South Jordan, Draper, and Salt Lake City.
The next best step is a thorough exam so we can determine whether your symptoms are truly plantar fasciitis, identify what is causing it, and help you start the right treatment from day one.
Ready to stop guessing and start improving?
IT Band Syndrome Rehabilitation: Phase 2
Once you progress through the first phase of rehab in our office, this video is a demonstrated of what you can be expected to work on at home. This is a mid-stage set of exercises - you do not start here.
5-min Running Warm-Up:
Every good run starts with a great warm-up.
“The team at Revive Sport & Spine has been SO helpful with my various running aches and pains. I really appreciate seeing providers who are athletes themselves and understand that I’m looking to optimize performance and push myself. Techniques like dry needling and shockwave therapy have been super helpful for my tight muscles and some nagging soft tissue injuries; Dr. Reheisse is very thoughtful in recommending the right treatment for different issues and trying different methods to get to the root of a problem. Highly recommend!”
“I cannot say enough good things about Revive and the amazing staff there! I am grateful that a friend referred me when I mentioned an Achilles issue I was dealing with. Dr. Reheisse is a runner himself, and extremely knowledgeable about and effective at treating running injuries. In-office treatment was helpful, and the at-home assignments were spot on for what I needed. He also helped give me the knowledge to continue progressing my rehab as time goes on.”